Chronic low back pain: what to do when back pain persists
What is chronic low back pain?
Chronic low back pain corresponds to pain localised in the lumbar region, persisting for more than three months. In the majority of cases, it is described as non-specific (85% of cases), meaning that no serious pathology or major structural lesion is identified on medical imaging.
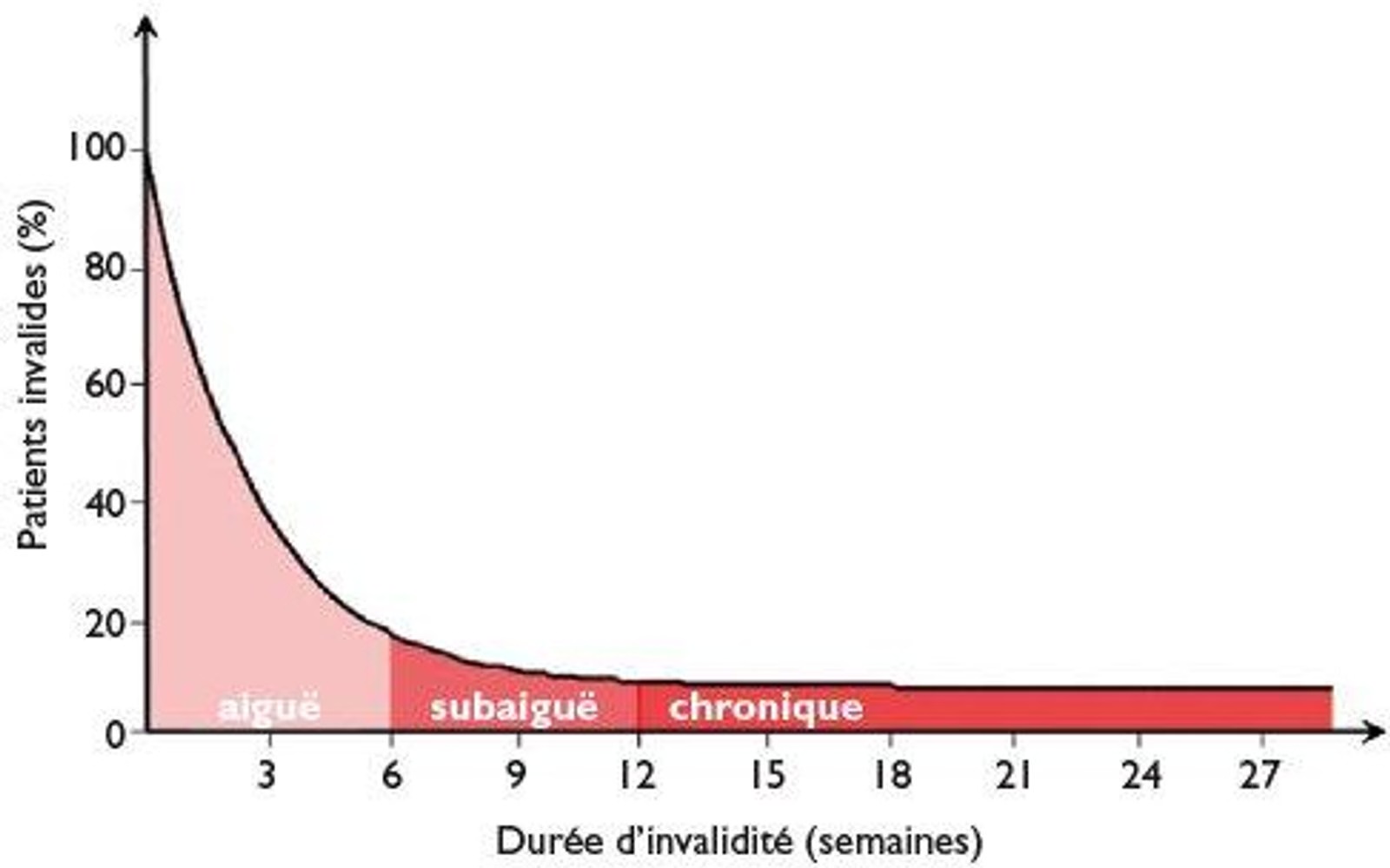
Low back pain is today a major public health issue worldwide. According to the main international epidemiological studies, back pain is the leading cause of disability in the world, ahead of many chronic diseases.
It is estimated that approximately 619 million people suffered from low back pain in 2020, and that this figure could exceed 840 million by 2050, under the combined effect of population ageing, sedentary behaviour and changes in occupational demands.
Although the majority of lumbar episodes are acute and transient, a significant proportion progresses to a persistent form. Data show that approximately 10% of people with low back pain develop chronic low back pain, defined as pain lasting more than three months.
- A significant reduction in quality of life.
- Lasting functional limitations.
- High occupational absenteeism.
- A major socio-economic cost for healthcare systems.
These figures underline the importance of effective, durable and scientifically grounded management, going beyond a purely symptomatic approach.
Why does back pain become chronic?
Contrary to received ideas, the absence of serious visible abnormality does not mean that the pain is "imaginary". It often reflects a complex dysfunction of the musculoskeletal and neurological systems, involving:
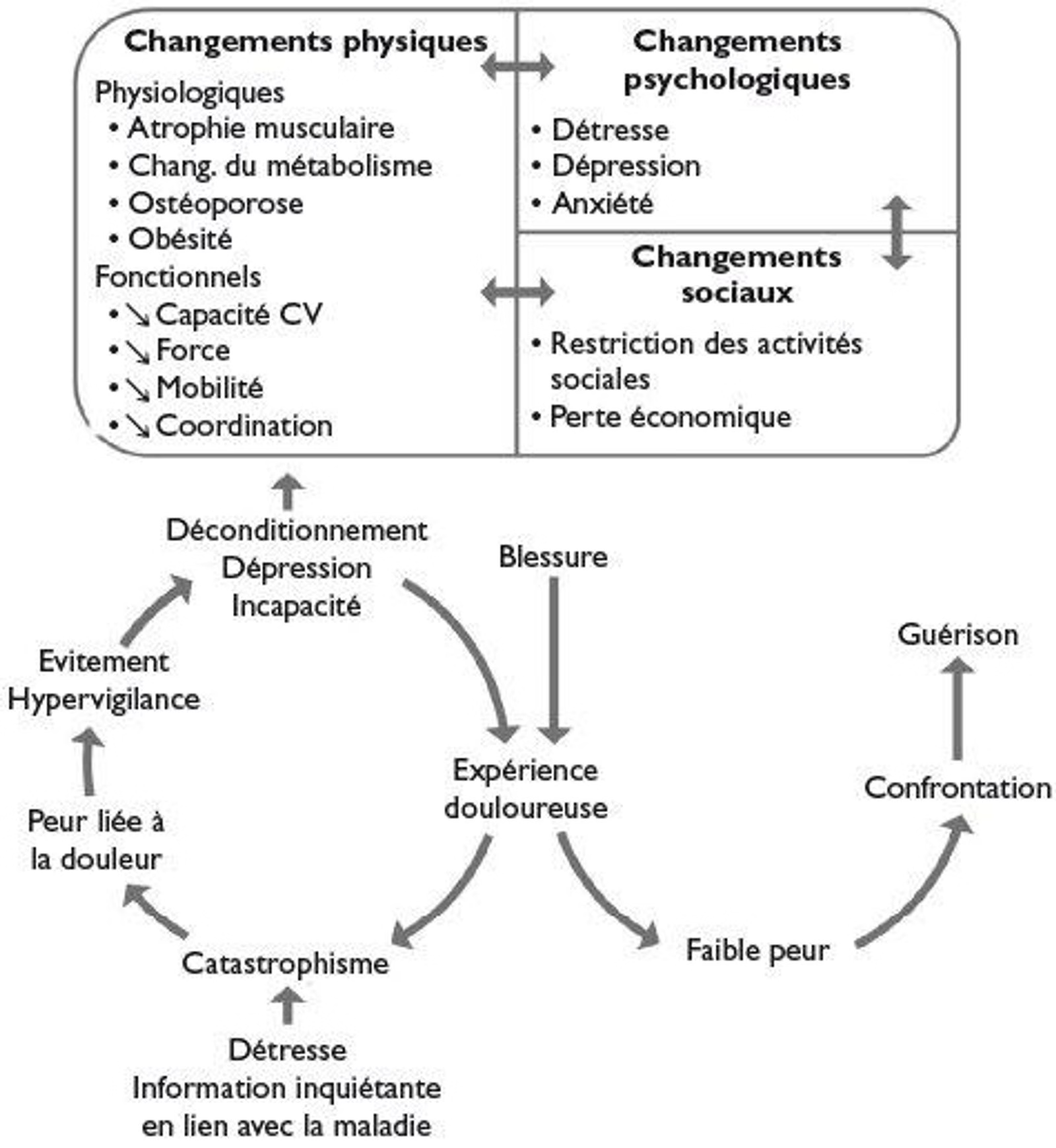
- Muscular weakness.
- Altered joint mobility.
- Ineffective postural adaptations.
- Psychosocial and environmental factors.
- Alterations in pain pathways (pain centralisation).
- Low-grade inflammation.
Chronic low back pain should therefore be understood as a multifactorial disorder, and not as a simple local problem of the back.
The role of osteopathy and manual therapy in chronic low back pain
Manual techniques aim to:
- reduce excessive tensions,
- improve joint mobility,
- optimise movement coordination,
- decrease mechanical loads on the lumbar region.
The objective is not solely immediate relief, but the creation of conditions favourable to lasting functional recovery.
Scientific recommendations for chronic pain
Recent scientific data, as well as the recommendations of the World Health Organization, confirm that manual therapies have a beneficial short-term effect in patients with non-specific chronic low back pain, notably by reducing pain intensity and moderately improving function.
However, systematic reviews also highlight an essential point:
- the effects of manual therapies alone tend to diminish over time when not combined with active strategies.
Current literature converges towards a so-called multimodal approach, combining:
- Manual therapy.
- Adapted therapeutic exercise and muscular strengthening.
- Patient education.
- Management of psychological and social factors influencing pain.
This integrated approach is today considered the most relevant for durably improving chronic low back pain.
-(Falcon, A., & Latanger, I. The effectiveness of manual therapy in people with chronic non-specific low back pain: an umbrella review with meta-analysis. Annals of Physical and Rehabilitation Medicine, 69(2), 102049, 2026).
-https://www.who.int/news/item/07-12-2023-who-releases-guidelines-on-chronic-low-back-pain
A comprehensive, active approach grounded in scientific recommendations
Within this framework, the management proposed rests on a solid scientific basis and a modern vision of chronic pain.
- A thorough functional evaluation,
- Manual techniques adapted to the patient's profile,
- Specific muscular strengthening programmes, targeting the muscles of the trunk, pelvis and hips,
- Progressive work on load and movement tolerance,
- Individualised advice based on current data concerning physical activity and recovery.
The objective is twofold:
- Reduce pain,
- Above all, restore durable function and prevent recurrence.
Chronic low back pain is thus addressed as a complex functional imbalance, requiring a structured, evolving and personalised strategy.
My practice is specifically oriented towards the management of chronic pain, and in particular chronic low back pain. My university and post-graduate training in osteopathy, neuroscience of movement and pain management allow me to approach this type of pain with a comprehensive, current and evidence-based vision.
Conclusion
Chronic low back pain is neither an inevitability, nor a simple local problem of the back. It reflects a multifactorial imbalance, requiring a comprehensive, active approach grounded in current scientific data.
A strategy combining manual therapy, specific strengthening, movement and education constitutes today the most coherent approach to durably improving pain, function and quality of life.
Osteopath - Chronic pain management - Sport
French Diploma of Osteopathy
Frequently asked questions (FAQ)
What is chronic low back pain?
Chronic low back pain is pain in the lower back persisting for more than 3 months. It accounts for 85% of low back pain cases and results from a combination of mechanical, neurobiological and psychosocial factors (biopsychosocial model).
Is osteopathy effective for chronic low back pain?
Yes, osteopathy is recommended in HAS guidelines for non-specific chronic low back pain. It reduces pain, improves mobility and decreases analgesic use according to several randomised trials.
What are the management strategies for chronic low back pain?
Optimal management is multimodal: osteopathy, therapeutic exercise (strengthening, yoga), pain education, stress management and, if necessary, psychological support (CBT). Physical activity remains the cornerstone of treatment.
Why does chronic low back pain persist despite treatment?
Chronification often results from central sensitisation: the nervous system amplifies pain signals even in the absence of active tissue damage. Therapeutic education and cognitive-behavioural approaches are essential to break this cycle.