Chronic Pain
Myofascial syndrome: chronic muscular pain
Management by Charbel Kortbawi, osteopath in Paris 16, at the Cabinet Victor Hugo — 7 rue Georges Ville (75016).
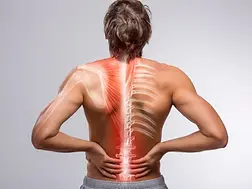
Definition and symptoms of myofascial syndrome
What is myofascial syndrome?
Myofascial syndrome is a chronic pain syndrome of the musculoskeletal system characterised by trigger points (TP): small zones of hyperexcitability nestled within a taut muscle band. When stimulated — by pressure, traction or sometimes spontaneously — these points provoke local pain which can radiate to other regions.
Doctors Janet Travell and David Simons, pioneers from the 1950s onwards, formalised the concept of TPs: a hypersensitive zone within an indurated muscle, capable of triggering a specific referred pain for the muscle concerned. They distinguish:
- Active TP: painful at rest or on exertion, it reproduces the typical referred pain of the muscle.
- Latent TP: clinically silent as long as it is not stimulated; pain only appears on provocation.
Although myofascial syndrome can be confused with other chronic conditions such as fibromyalgia, it is distinguished from them by the presence of genuine palpable trigger points and pain that is often more localised.
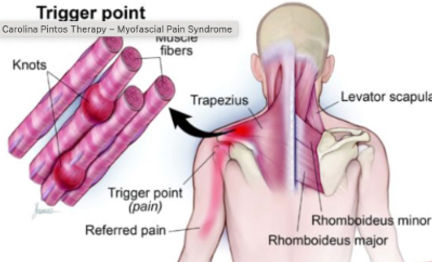
Symptoms of myofascial syndrome
The main symptoms include:
- Localised muscular pain: frequently felt in the neck, shoulders or back
- Active trigger points: sensitive muscular zones that trigger radiating pain when stimulated
- Muscular-origin stiffness
- Fatigue, sleep disturbances
- Headaches
- Postural imbalances
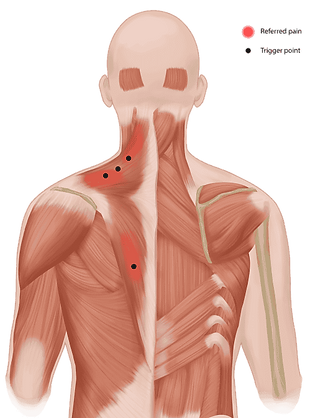
Diagnosis of myofascial syndrome
Clinical diagnosis
The diagnosis is based on a thorough clinical evaluation, as there are no specific imaging tests. The steps include:
- Detailed history: frequency, intensity, triggering and relieving factors of the pain
- Imaging investigations: as needed, to rule out other pathologies
- Observation: detection of postural abnormalities and imbalances
- Physical examination: searching for taut muscle bands and trigger points
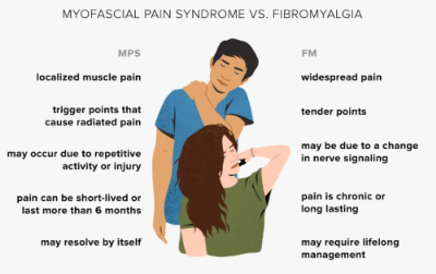
Difference between myofascial syndrome and fibromyalgia
- Myofascial syndrome: localised and regional pain accompanied by trigger points. Once treated, the pain disappears.
- Fibromyalgia: widespread pain throughout the body, chronic. Fatigue and sleep disturbances are very common.
It is possible for a person to suffer from both conditions simultaneously, making an accurate diagnosis essential.
Treatment of myofascial syndrome
Specific injection techniques
The injection of local anaesthetics or corticosteroids into trigger points temporarily numbs the painful zone, reducing local inflammation and thus relieving the immediate pain. These injections are often combined with other techniques to release muscular tension.
Dry Needling
Dry Needling (or "dry acupuncture") consists of inserting fine needles directly into the trigger points of the muscle. This method is effective in relieving muscular pain, reducing tension and improving muscular function.
Osteopathy and manual therapy
Osteopathy plays an essential role in the treatment of myofascial syndrome by offering a targeted manual approach. The osteopath uses manual techniques to:
- Inhibit trigger points: relax the muscles affected by trigger points
- Improve blood circulation: promote better oxygenation of muscular tissues
- Restore postural balance: identify and correct the imbalances that contribute to the development of the syndrome
Stretching, mobilisation and self-rehabilitation
Muscular stretches and mobilisations help to release tight muscles and improve flexibility. Patient education and the integration of self-exercises enable better management of pain on a daily basis and prevent recurrence.
Advantages of osteopathy in the treatment of myofascial syndrome
- Targeted action on trigger points: ischaemic compression inhibition techniques directly release the trigger points responsible for referred pain. It is the least invasive treatment for myofascial syndrome.
- Normalisation of articular mobility: through gentle manipulations (fascial, muscle energy, adapted HVLA techniques), the osteopath restores the mobility of adjacent joints, reducing the tension that maintains the trigger points.
- Comprehensive approach to the patient: myofascial syndrome is never isolated. Posture, stress, sleep disturbances or repetitive movements may fuel it. A qualified osteopath explores these factors to provide an adapted response.
- Therapeutic education and ergonomic advice: specific stretching exercises, postural advice at the office, load distribution during sport. This education reinforces the patient's autonomy.
Frequently Asked Questions
FAQ
What is a trigger point and how does osteopathy treat it?
A trigger point is a hyper-irritated zone within a muscle that causes local and referred pain. The osteopath treats them using ischaemic compression, myofascial stretching and post-isometric relaxation techniques, making it possible to deactivate these painful areas.
What is the difference between fibromyalgia and myofascial syndrome?
Fibromyalgia is a generalised condition with widespread pain, chronic fatigue and sleep disturbances. Myofascial syndrome is localised to specific muscles with identifiable trigger points. Both conditions can coexist but require different therapeutic approaches.
How many sessions to treat myofascial syndrome?
For an acute or recent myofascial syndrome, 3 to 5 sessions are generally enough. In chronic forms with numerous active trigger points, 6 to 10 sessions are needed, combined with a daily home stretching programme to maintain the results.
Which muscles are most often affected by myofascial syndrome?
The most frequently affected muscles are: the trapezius and the levator scapulae (neck pain and headaches), the quadratus lumborum (low back pain), the piriformis and the gluteal muscles (sciatica), the sternocleidomastoid (dizziness, facial pain) and the masticatory muscles (jaw pain).