Chronic Pain
Irritable bowel syndrome: osteopathy and manual therapy to relieve digestive disorders
Care provided by Charbel Kortbawi, osteopath in Paris 16, at Cabinet Victor Hugo — 7 rue Georges Ville (75116).
Irritable bowel syndrome: causes and features
Definition
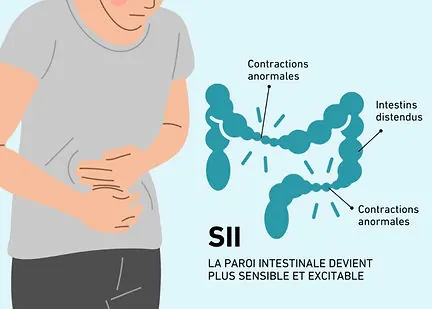
Irritable bowel syndrome (IBS) is a common gastrointestinal disorder that affects millions of people worldwide. It is classified as a functional condition, because there is no visible lesion of the bowel, but rather abnormalities in its functioning. IBS is characterised by a complex interaction between the gut, the brain and the intestinal microbiota, and is influenced by psychological, nervous and environmental factors.

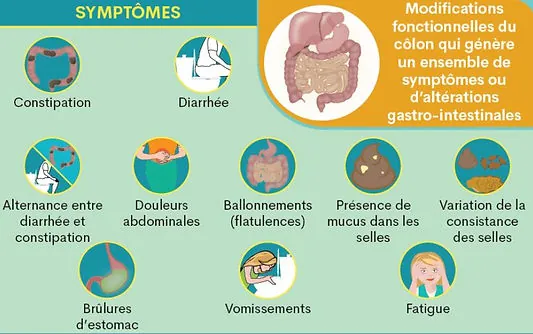
Common symptoms of irritable bowel syndrome
- Abdominal pain: often cramps or discomfort that can be relieved after a bowel movement.
- Bowel transit disturbances: alternation of diarrhoea and constipation, or predominance of one or the other.
- Bloating and gas: a sensation of abdominal swelling that can be exacerbated by certain foods.
- Fatigue and headaches: less frequent symptoms, but which may be present due to the general discomfort.
These symptoms may appear in episodes or be constant, and are often aggravated by stress, certain foods or previous gastrointestinal infections.
Diagnosis of irritable bowel syndrome (Rome IV criteria)
Recurrent abdominal pain at least once a week during the last three months, associated with at least two of the following features:
- The pain is related to defecation
- A change in the frequency of stools
- A change in the consistency of stools
Exclusion of other causes: doctors may carry out tests to rule out other conditions (inflammatory bowel disease, coeliac disease, infections, colon cancer in patients > 50 years).
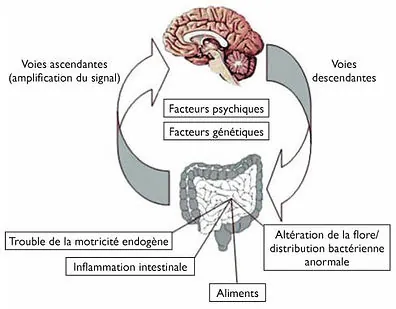
Pathophysiological mechanisms
Link between emotional state and intestinal symptoms: IBS appears to be part of the continuous reaction of the digestive tract and central nervous system (CNS) to internal and external stimuli. Psychological factors (depression, anxiety) can influence communication between the CNS and the enteric nervous system.
Disturbance of intestinal motility: patients with IBS show a decreased expression of specific serotonin reuptake transporters (SERT), with consistently raised serotonin levels and dysregulation of intestinal motility.
Visceral hypersensitivity: increased perception of stimuli, likely a consequence of amplification of nociceptive signals in the CNS.
Intestinal inflammation: increased intestinal immune response with elevated plasma levels of pro-inflammatory cytokines.
Alteration of the gut flora and genetic factors.
Treatment of irritable bowel syndrome
IBS has no curative treatment, but several approaches can reduce symptoms. Treatment is often multimodal:
Dietary modifications
- Low-FODMAP diet: fermentable carbohydrates which worsen symptoms. Can reduce bloating.
- Fibre supplementation: soluble fibres (psyllium) recommended in case of constipation.
Medication
- Antispasmodics to reduce cramps
- Laxatives or antidiarrhoeals depending on the form of IBS
- Probiotics with beneficial effects on the microbiota
Psychological therapies
- Cognitive behavioural therapy (CBT): helps manage triggers of stress and anxiety
- Hypnotherapy: may reduce visceral hypersensitivity
Physical activity
Regular exercise is associated with improved intestinal motility and reduced stress.

Contribution of osteopathy in the treatment of irritable bowel syndrome
Pain reduction and improvement in quality of life
Research on the effect of osteopathic sessions on irritable bowel syndrome indicates a significant improvement: osteopathic treatments reduce symptoms such as abdominal pain and bloating, and improve patients' quality of life. Several studies show that visceral osteopathy, by working on the mobility of the viscera, helps reduce spasms and improves intestinal motility. The soothing effects of osteopathy on the nervous system also help to alleviate fatigue and anxiety. Moreover, research has shown that osteopathy is safe and has no side effects. (Buffone et al., 2023; Hundscheid et al., 2007; Florance et al., 2013; Muller et al., 2014)
Frequently Asked Questions
FAQ
Is osteopathy effective for irritable bowel syndrome?
Several clinical studies show the effectiveness of visceral osteopathy in irritable bowel syndrome (IBS). Abdominal techniques reduce pain, bloating and improve transit. Results are optimal when combined with dietary follow-up and stress management.
How many sessions are needed to improve irritable bowel syndrome?
On average, 4 to 6 sessions spaced 3 to 4 weeks apart allow a significant improvement in symptoms. Some patients feel an improvement from the 2nd session. A quarterly maintenance consultation is then recommended to preserve the results.
What osteopathic techniques are used for IBS?
The osteopath mainly uses visceral techniques (gentle mobilisation of the digestive organs, colon, small intestine), structural techniques on the lumbar spine and diaphragm, and cranial techniques to regulate the autonomic nervous system involved in intestinal motility.
Does stress aggravate irritable bowel syndrome and what can be done about it?
Yes, stress is a major aggravating factor in IBS via the gut-brain axis. Osteopathy acts indirectly on stress by regulating the autonomic nervous system. In addition, heart-coherence techniques, meditation and an adapted lifestyle are recommended.