Temporomandibular disorders
Management of chronic jaw pain in Paris 16
Understanding chronic jaw pain
Definition and epidemiology
Chronic pain of the temporomandibular joint (TMJ) is the second most common cause of chronic musculoskeletal pain after low back pain, affecting 6 to 9% of adults worldwide. It manifests as pain in the jaw and associated structures, as well as symptoms such as headaches, ear pain, noises or crepitus in the temporomandibular joint, and impaired mandibular function. Chronic pain is defined as pain that has been present for more than 3 months.
What are the causes?
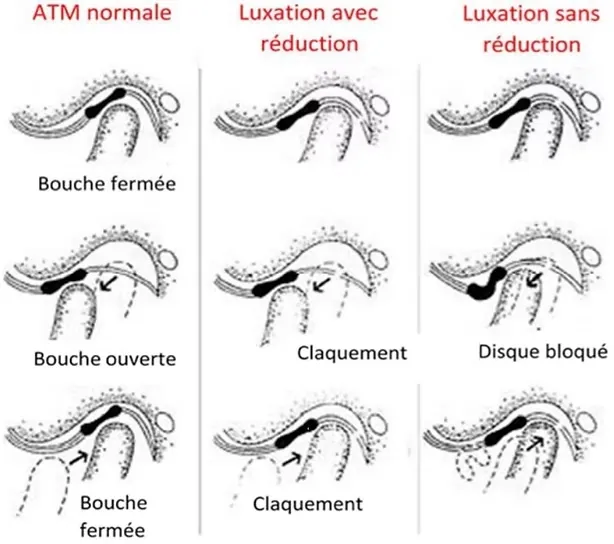
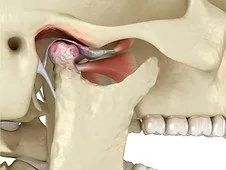
- Temporomandibular dysfunction (disc displacement, osteoarthritis)
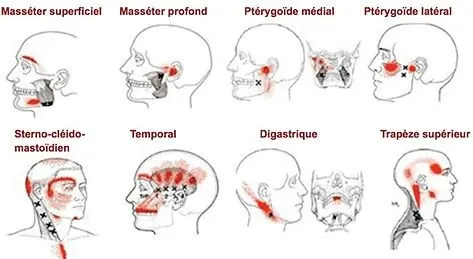
- Myofascial syndrome (bruxism, clenching): muscular overuse creating painful trigger points
- Direct or repetitive trauma (prolonged dental surgery, cervical or facial impact)
- Systemic inflammatory conditions (rheumatoid arthritis, spondyloarthritis) that may affect the TMJ
These sustained aggressions lead to central sensitisation: the nervous system lowers its nociceptive threshold and amplifies every stimulus. On top of this biological basis, psychological and social factors are added: stress, anxiety, depression, work overload, disturbed sleep or lack of social support.
Symptoms of jaw pain
- Pain in front of the ear
- Pain in the jaw
- Pain in the masticatory muscles
- Headaches
- Joint noises (clicking, grating)
- Limited mouth opening
- Tinnitus

Treatment of chronic jaw pain
The latest recommendations published in the BMJ (British Medical Journal) in December 2023
Strong recommendations in favour:
- Cognitive behavioural therapy (CBT)
- Passive mobilisations of the joint
- Postural exercises
- Exercises and stretches of the TMJ muscles
- Trigger point therapy
- Usual care
Conditional recommendations in favour:
- Manipulation
- Non-steroidal anti-inflammatory drugs + CBT
- Acupuncture
- Exercises + joint mobilisations

Treatment with osteopathy and manual therapy in Paris 16
This management fits into our overall approach to chronic musculoskeletal pain.
Scientifically proven efficacy of osteopathic treatment
Osteopathy and manual therapy are approaches that have scientifically demonstrated their efficacy in the management of chronic jaw pain, and have shown a significant reduction in pain and an improvement in patients' quality of life. Osteopathic techniques include specific and safe manual techniques to release the muscles of the temporomandibular joint, as well as those of the neck.
Mr Charbel Jean Kortbawi DO, MSc, osteopath specialising in pain management, treats acute and chronic pain of the temporomandibular joint at his practice in Paris 16.
Frequently Asked Questions (FAQ)
How many sessions are needed for jaw pain?
Generally, 4 to 6 sessions are needed for chronic TMJ pain. Acute pain may respond in 2 to 3 sessions. Coordinating with the dentist (occlusal splint) significantly improves outcomes.
Should I see a dentist or an osteopath for jaw pain?
Both approaches are complementary. The dentist treats the occlusal components (splint, dental adjustment). The osteopath works on the muscular and articular components. Coordinated management is recommended by experts in line with the BMJ 2023 recommendations.
Can osteopathy help with night-time bruxism?
Osteopathy reduces the muscular tension linked to bruxism (masseter, temporalis, pterygoid muscles) and can decrease the frequency of episodes. It does not treat the psychological component of bruxism, for which CBT is recommended.
What are the symptoms of TMJ disorders?
Symptoms include: pain in front of the ear, limited mouth opening, joint noises (clicking, grating), headaches, associated neck pain and sometimes tinnitus. These symptoms may be unilateral or bilateral.
Related articles