Chronic Pain
How to relieve chronic pain with an osteopath in Paris 16
What is chronic pain?
According to the IASP (International Association for the Study of Pain), “pain is an unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage.”
- The term sensory means that pain can be described in terms of its physiological characteristics.
- The term emotional underlines that pain is unpleasant and subjective.
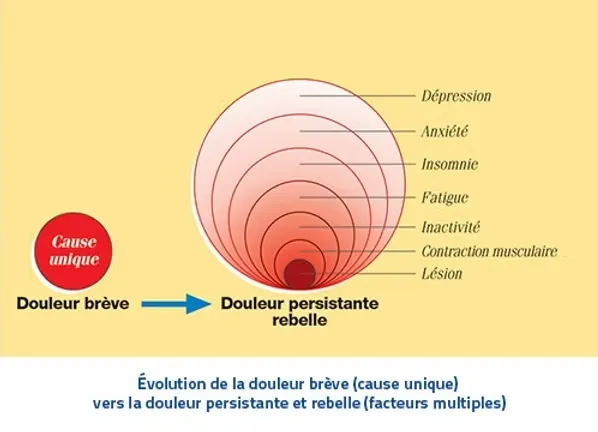
Pain functions as an alarm signal. If acute pain persists beyond three months, it evolves into chronic pain. At that point, the sensation loses its meaning as an alarm signal: pain is no longer a symptom but becomes a disease in its own right.

Characteristics of chronic pain
1) Persistence over time
Chronic pain is defined above all by its duration. It persists well beyond the expected healing time, generally for more than three to six months. This persistence reflects a change in pain-regulation mechanisms, which no longer disappear even once the initial lesion has healed.
2) Independence from the initial stimulus
Over time, pain can become independent of its initial cause. Even in the absence of active tissue damage or an inflammatory process, pain continues to be perceived. This is explained by changes in the nervous system, which sustains the pain signal autonomously.
3) Emotional modulation
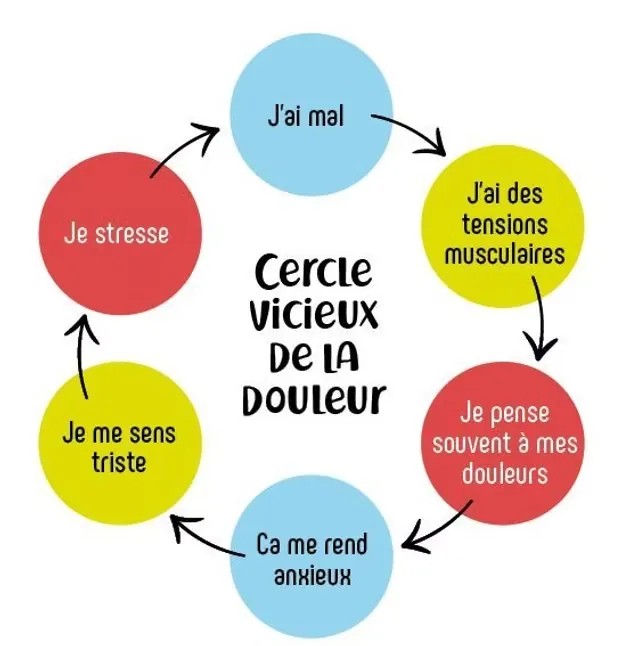
Chronic pain is strongly influenced by emotional factors. Stress, anxiety or depression can amplify the perception of pain. Conversely, certain positive psychological factors can contribute to reducing it, illustrating the close link between the brain and pain perception.
4) Central sensitisation
The central nervous system becomes progressively more sensitive. This is referred to as central sensitisation, where stimuli that would normally be non-painful are perceived as painful, or where pain is amplified disproportionately. This phenomenon plays a key role in many chronic pain conditions.
5) Functional impairment
Chronic pain has a direct impact on quality of life. It can lead to reduced physical capacity, limitation of daily activities, and an impact on sleep, work and social life. This functional impairment often contributes to maintaining the vicious cycle of pain.
How does pain become chronic?
1) Biological factors
Nerve damage or neuropathic lesions: damage to the nervous system, as in neuropathic pain (e.g. diabetic neuropathy, post-herpetic neuralgia), can lead to persistent pain.
2) Prolonged inflammation
Chronic inflammatory diseases, such as arthritis or fibromyalgia, can perpetuate pain through continuous activation of nociceptors (pain receptors).
3) Neuronal plasticity
Long-lasting changes in pain processing at the neuronal circuit level, such as hyperexcitability of spinal cord neurons or loss of natural inhibitory mechanisms, can maintain pain.
4) Psychological factors
- Stress and anxiety: chronic stress or anxiety are major factors in the transition to chronic pain.
- Depression: depression is frequently associated with chronic pain, both as a consequence and as an aggravating factor.
- Catastrophising: a tendency to exaggerate the negative consequences of pain can reinforce sensitisation pathways.
5) Social factors
Social isolation: a lack of social support can worsen chronic pain.
6) Economic factors
Unemployment or financial problems can create a vicious cycle.
7) Behavioural factors
Physical inactivity and self-medication can sustain pain.
Osteopathy and the management of chronic pain
Osteopathy is recognised for its effectiveness in the management of chronic pain, particularly through non-invasive manual approaches aimed at restoring the structural and functional balance of the various body systems. Charbel Kortbawi, osteopath in Paris 16, consults at the Victor Hugo practice for the personalised management of chronic pain.
This global action promotes modulation of nociceptive pathways, a calming of sympathetic over-activity and a reduction in the phenomena of central sensitisation.
The main syndromes treated
Low back pain
Chronic lumbago
Learn moreFibromyalgia
Diffuse chronic pain
Learn moreHeadaches and migraines
Chronic tension headaches
Learn moreIrritable bowel syndrome
Functional bowel disorders
Learn moreChronic pelvic pain
Pelvis and endometriosis
Learn moreJaw pain
TMJ disorders, bruxism
Learn moreMyofascial syndrome
Trigger points, deep tension
Learn moreCharbel J. Kortbawi, osteopath specialising in chronic pain in Paris 16
Pain chronification is a multifactorial process combining biological, psychological and social dimensions. Mr Charbel Kortbawi holds the following qualifications:
- University Diploma “Chronic Pain Management” (Université Paris-Sorbonne)
- University Diploma “Pain and Human Motor Function” (Université Polytechnique Hauts-de-France)
- Master 2 in Neurosciences
Further reading: the placebo effect in pain management, and cervicogenic dizziness explained.
Frequently Asked Questions (FAQ)
What is chronic pain and how can an osteopath in Paris 16 help?
Chronic pain persists beyond 3 months, often in the absence of an active lesion. It involves central sensitisation mechanisms. Osteopathy acts on the mechanical components (muscular tension, joint restrictions), reducing nociceptive signals and improving quality of life.
How many sessions are needed to see an improvement with an osteopath in Paris 16?
For chronic pain, initial improvements are generally seen after 3 to 4 sessions. A complete protocol often comprises 6 to 10 sessions over 3 to 6 months, depending on the complexity and duration of the pain. Osteopathy is most effective when combined with a tailored exercise programme.
Is osteopathy reimbursed by the French social security for chronic pain?
Osteopathy is not reimbursed by the French Assurance Maladie. However, many complementary health insurance policies cover 1 to 4 sessions per year. Please check with your provider. The rate for a session at the Victor Hugo practice in Paris 16 is available on the contact page.
Which chronic pain conditions are most commonly treated by an osteopath in Paris 16?
The conditions most frequently managed are: chronic low back pain, fibromyalgia, chronic headaches, irritable bowel syndrome and myofascial syndrome. A personalised approach is established for each patient.