Placebo effect and chronic pain
What is the placebo effect?
The placebo effect is the therapeutic effect obtained by the administration of tablets, liquids, injections and any procedures that have no specific effect on the disease being treated. The placebo effect is a complex phenomenon that rests on sophisticated neurophysiological mechanisms, particularly with regard to pain management. Although the placebo contains no active substance, it can provoke significant changes in the neuronal networks involved in the perception and modulation of pain.
Neurophysiological effects of the placebo effect
When a placebo is administered to an individual suffering from pain, certain areas of the brain — such as the dorsolateral prefrontal cortex (DLPFC), the anterior cingulate cortex (ACC) and the insula — are activated. These regions are involved in pain modulation and in the anticipated expectations of pain relief. The DLPFC, for example, is essential for the management of expectations and decision-making, and plays a key role in the anticipation of relief. The ACC, often called the "emotional centre of pain", is responsible for the emotional component of pain. It is involved in the processing of the emotional suffering associated with pain, and it is activated in response to the administration of placebos, which suggests that expectations linked to relief can modulate this subjective component.
Effect on neurotransmitters
Another key mechanism of the placebo effect in pain management is the modulation of neurotransmitter systems. Studies have shown that placebo induces an increased release of endogenous endorphins, which are natural opiates produced by the brain. These endorphins bind to opioid receptors in various brain regions, such as the thalamus and the brainstem, and reduce the perception of pain. In other words, the administration of a placebo can activate the same neurochemical circuits as those targeted by opioid analgesics, without the actual administration of these drugs.
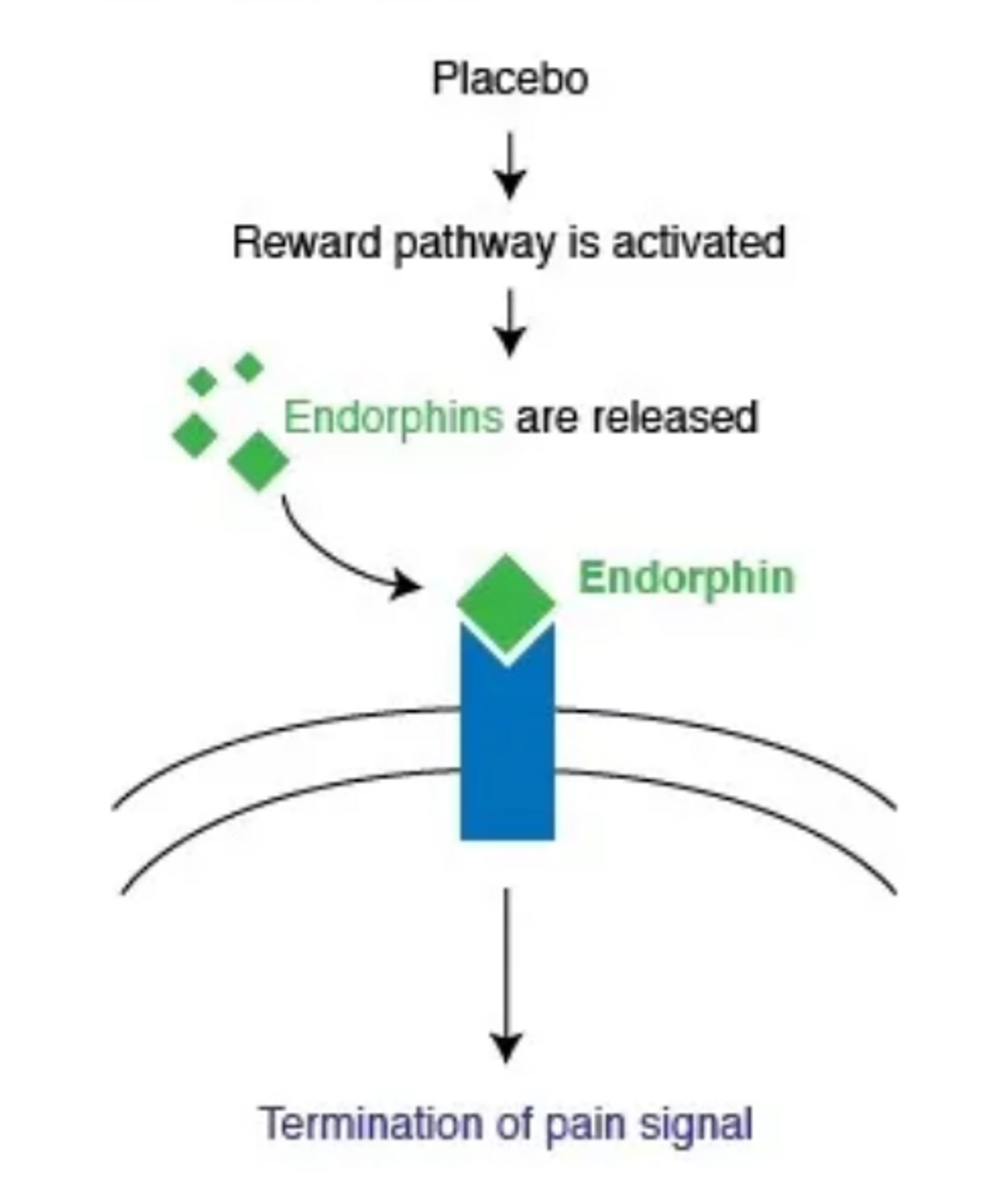
Dopaminergic networks and anticipation
The placebo effect also rests on the dopaminergic networks of the brain, notably within the reward system. The release of dopamine in the ventral striatum and the nucleus accumbens is an anticipatory response to the expected pain relief. These regions, generally associated with reward and pleasure, show increased activity when the patient expects an improvement in their condition, thereby amplifying the placebo effect.
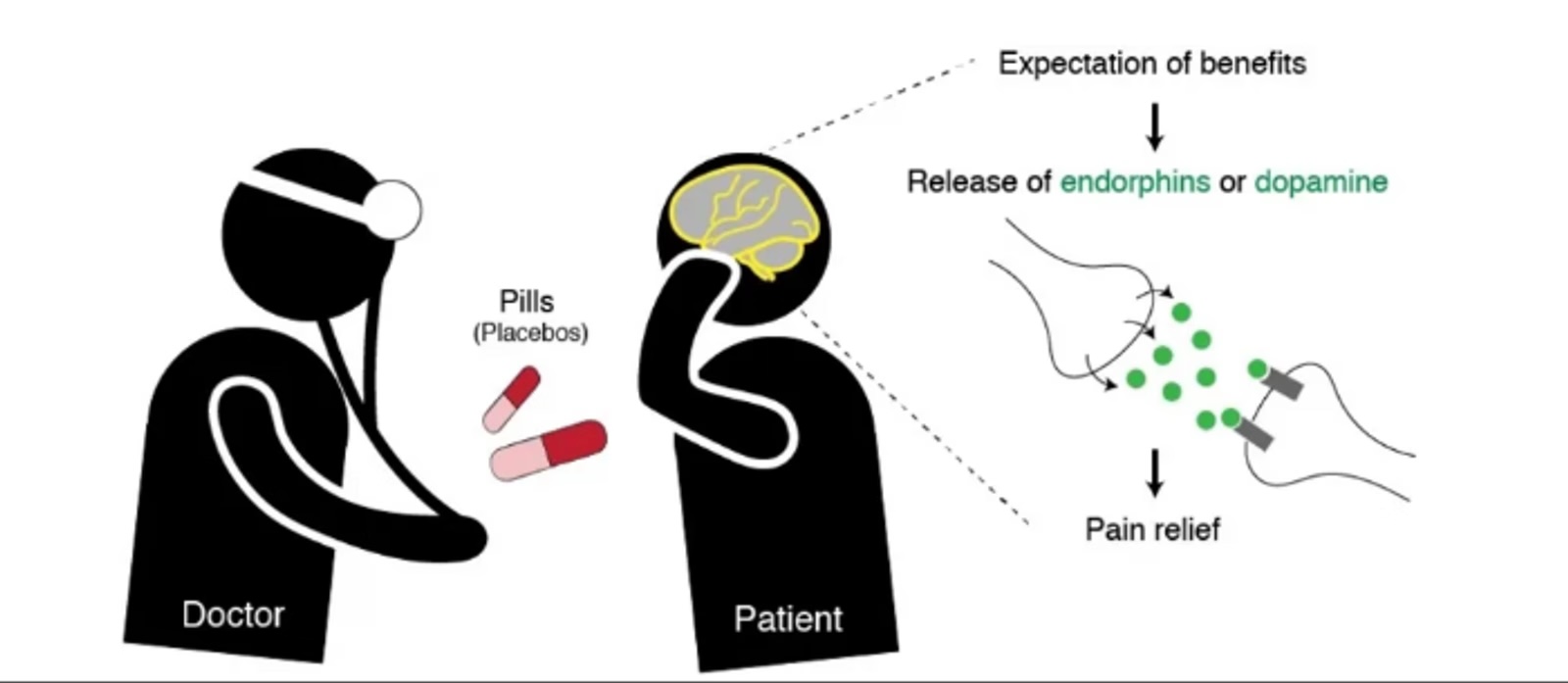
Persistence and variability of the placebo effect
The placebo effect can vary according to the expectations of patients, the context in which the treatment is administered, and even the type of pain. Recent studies in animal and human models have also revealed that the placebo effect is influenced by neuronal plasticity, that is, the capacity of the brain to reorganise its circuits in response to new experiences. This suggests that the placebo effect can evolve over time, notably in chronic patients who have been regularly exposed to medical interventions.
Conclusion
In conclusion, the placebo effect in pain management is not limited to a mere psychological illusion. It rests on a complex modulation of the neuronal networks involved in the perception of pain, expectations and emotions. Endorphins and dopamine play a key role in these processes, as do the cognitive and emotional circuits of the brain. Understanding these mechanisms can help to improve pain treatments and reduce the use of analgesics, notably in conditions of chronic pain.
Frequently asked questions (FAQ)
Does the placebo effect play a role in osteopathy?
The placebo effect is present in all treatments, including osteopathy. However, the real biological mechanisms of osteopathy (neuro-mechanical modulation, reduction of local inflammation) are well documented and distinct from the pure placebo effect.
What is the placebo effect in chronic pain?
The placebo effect is a reduction of pain induced by belief in a treatment, without any direct pharmacological or mechanical action. It mobilises real neurobiological mechanisms (endorphins, serotonin) and may represent 20 to 40% of the observed therapeutic effect.
Can the nocebo effect worsen chronic pain?
Yes, the nocebo effect is the opposite of the placebo: a negative belief about a treatment or one's condition can amplify pain. This is why therapeutic education and positive communication are essential in the management of chronic pain.
How do you distinguish the effect of a treatment from the placebo effect?
Only randomised controlled trials against placebo allow the specific effect of a treatment to be measured. For osteopathy, several randomised studies have shown effects superior to placebo for chronic low back and neck pain.