Treatment of chronic low back pain: a multimodal approach
Scientific recommendations for the treatment of chronic low back pain
Chronic low back pain is a major public health problem, affecting millions of people worldwide. It is the most frequent condition responsible for chronic pain, causing significant functional limitation and deterioration of patients' quality of life. The causes of non-specific chronic low back pain are not clearly defined. The treatments of this condition have been the subject of numerous recommendations around the world.
Scientific recommendations, notably those from the Haute Autorité de Santé (France), the National Institute of Health and Care Excellence (United Kingdom), and other health agencies in North America and Europe, converge towards similar approaches.
- Non-pharmacological treatments for chronic low back pain: Active exercise and rehabilitation
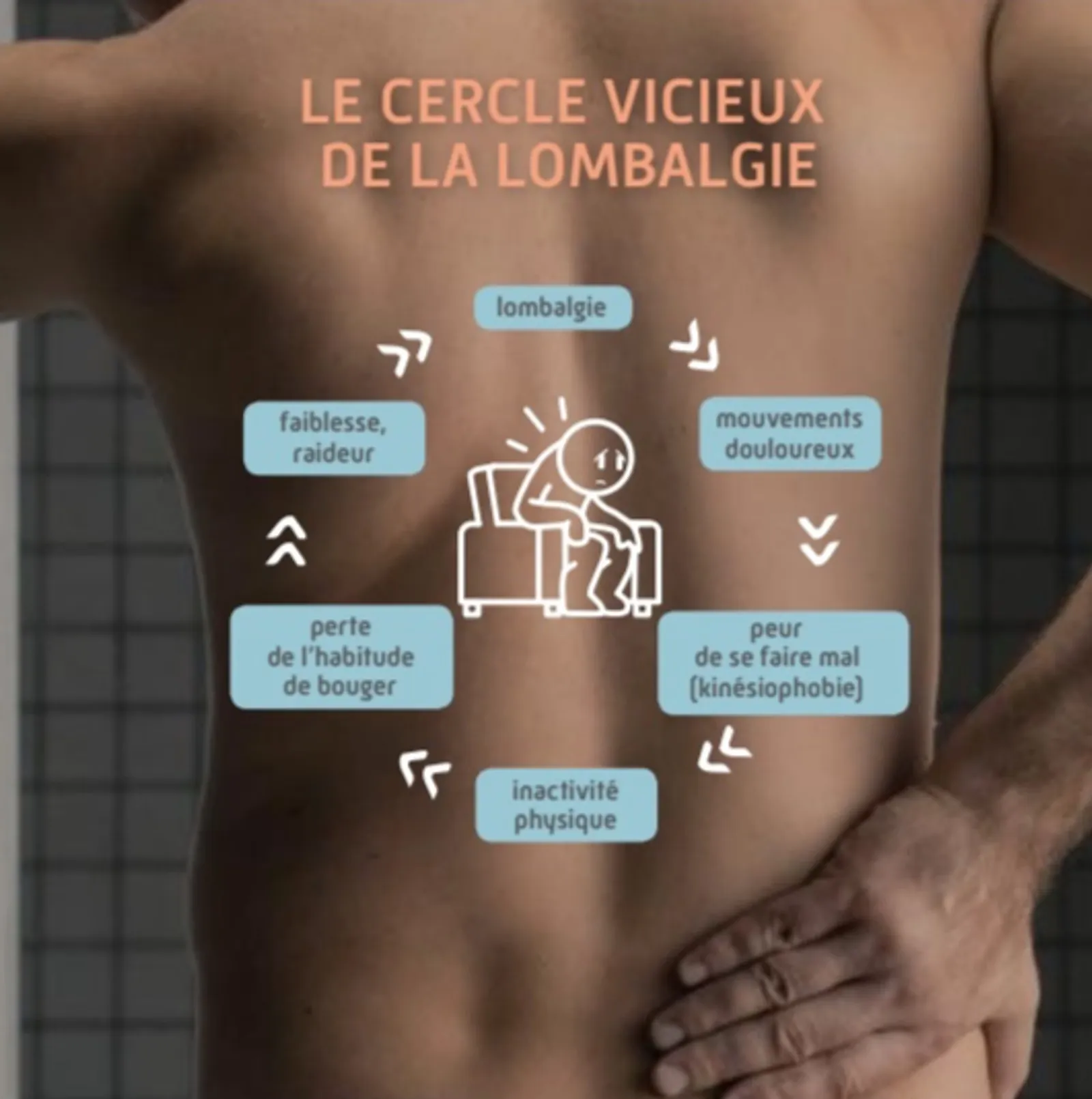
It is strongly recommended that the patient adopts an active rehabilitation programme, including adapted physical exercises. The objective is to promote movement and reduce sedentary behaviour, while allowing better management of pain.
- Manual therapy, mobilisations and manipulations — Osteopathy, chiropractic and other forms of manual therapies are advised in combination with a physical exercise programme. These approaches are particularly effective when integrated into multidisciplinary management.
- Patient education — Informing and educating the patient about the nature of chronic pain and the importance of physical activity is essential for long-term management.
- Psychotherapy (CBT) — Cognitive behavioural therapy is recommended, particularly when low back pain is associated with psychological disorders such as anxiety or depression.
- Pharmacological treatments for chronic low back pain: Non-steroidal anti-inflammatory drugs (NSAIDs)
These are often used as a first-line treatment to relieve acute pain, but their use must be of short duration.
- Antidepressants (Duloxetine)
In some cases, antidepressants such as duloxetine may be prescribed as a second-line treatment, particularly when pain is difficult to manage with anti-inflammatories.
- Opioids
Their long-term use is not recommended due to the risks of dependence, but may be considered as a third-line option in severe cases.
Conclusion
Corticosteroid injections, TENS, orthopaedic insoles and support belts or corsets have no consensus of use according to the scientific recommendations of several learned societies.
These approaches show the importance of comprehensive and personalised management, combining physical, psychological and sometimes pharmacological interventions. They aim to reduce pain, improve function and enable the patient to resume daily activities.
For anyone suffering from chronic low back pain, it is essential to consult a healthcare professional in order to follow a treatment adapted and based on the most recent scientific recommendations.
Frequently asked questions (FAQ)
What is the multimodal approach for chronic low back pain?
The multimodal approach combines: osteopathy for the mechanical components, therapeutic exercise (strengthening, yoga, Pilates), education in pain neurophysiology, and if necessary, psychological support (CBT). This combination gives the best results according to international guidelines.
Is osteopathy recommended for chronic low back pain?
Yes, the HAS (French National Authority for Health) recommends manual therapies, including osteopathy, in the management of non-specific chronic low back pain. Scientific evidence shows a reduction in pain and functional improvement.
Should I see a physiotherapist or an osteopath for chronic low back pain?
The two are complementary. Osteopathy treats joint and visceral dysfunctions, while physiotherapy focuses on muscular strengthening and functional rehabilitation. Coordinated management between the two practitioners optimises results.
How many osteopathy sessions to treat chronic low back pain?
A minimum of 6 to 10 sessions is recommended for chronic low back pain, combined with a daily exercise programme. The frequency is generally once a week at the start, then gradually spaced depending on clinical progress.