Piriformis syndrome : causes and treatment
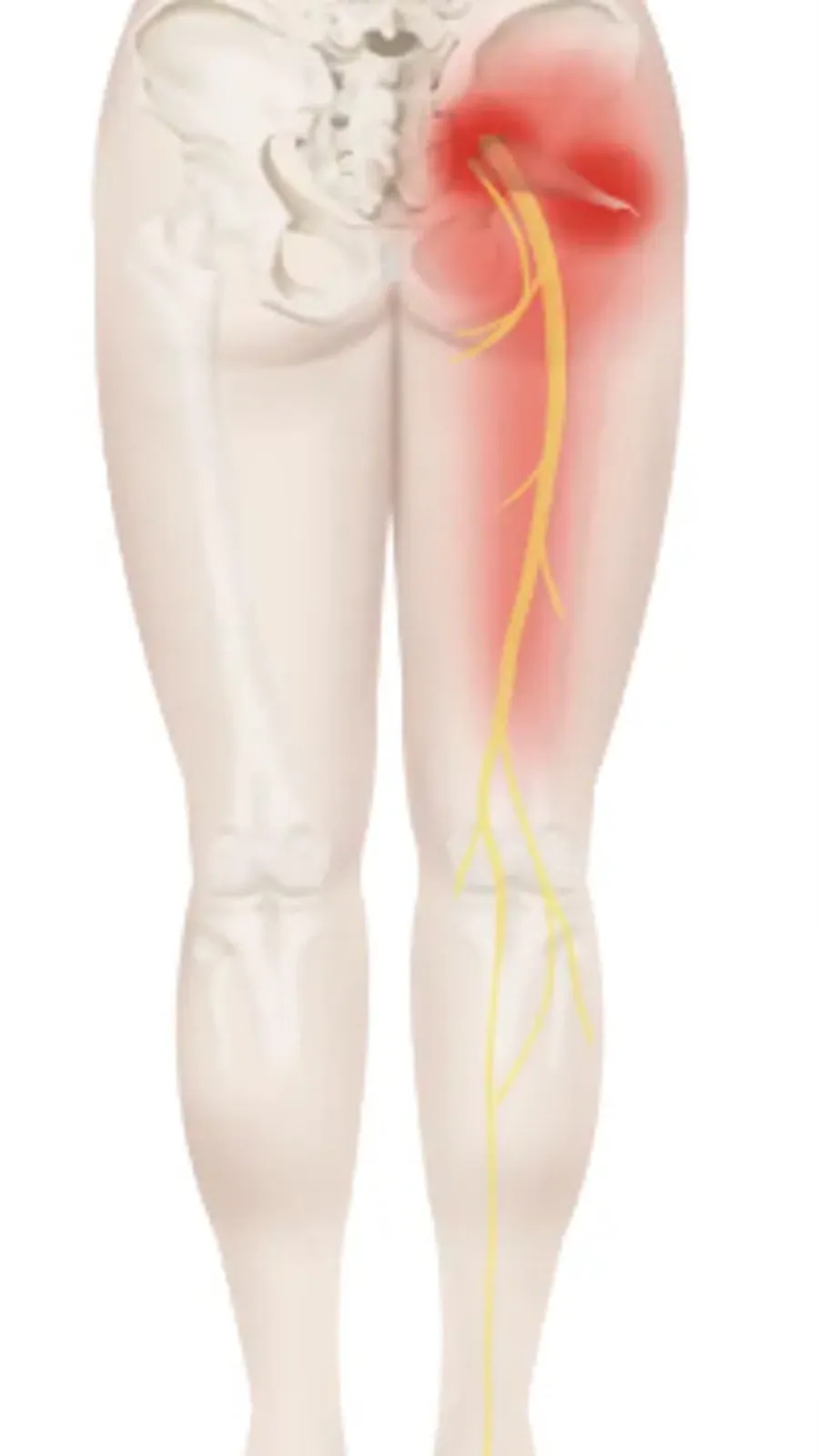
Piriformis muscle syndrome is a common and under-recognised cause of sciatica.
What is piriformis syndrome?
Piriformis muscle syndrome (PMS) is a neuromuscular disorder characterised by compression of the sciatic nerve by the piriformis muscle, located deep within the gluteal region. This pathology, though often under-recognised, may account for up to 6 to 8% of cases of sciatic pain. Patients typically present with buttock pain radiating into the thigh, mimicking sciatica of lumbar origin, sometimes with burning sensations, numbness or tingling along the course of the sciatic nerve.
Anatomy and role of the piriformis muscle
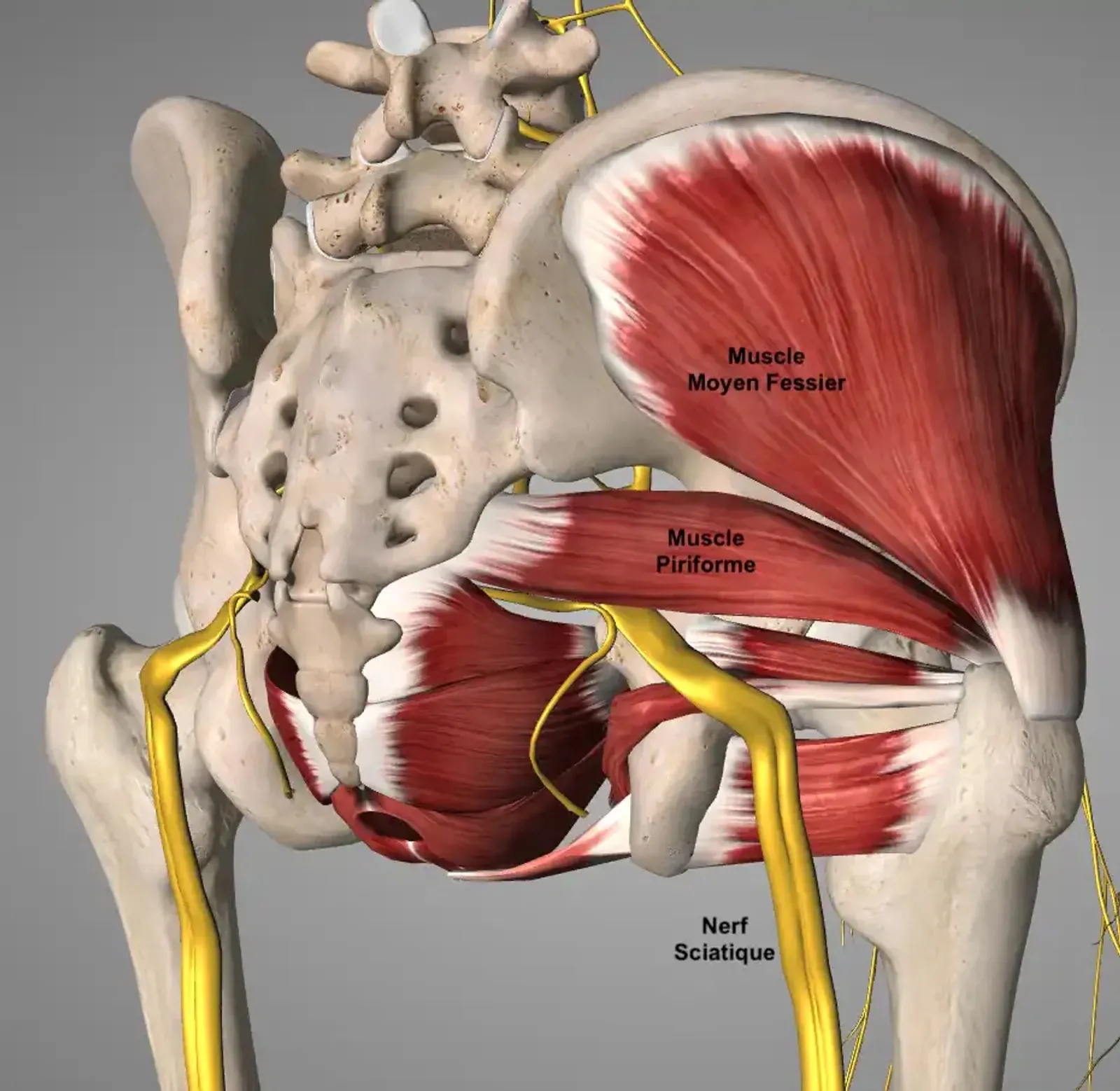
The piriformis muscle is a small, triangular, pear-shaped muscle originating from the anterior surface of the sacrum (S2–S4 foramina) and inserting on the upper border of the greater trochanter of the femur.
Its main functions are lateral rotation of the hip (with the hip extended), abduction (with the hip flexed) and hip extension.
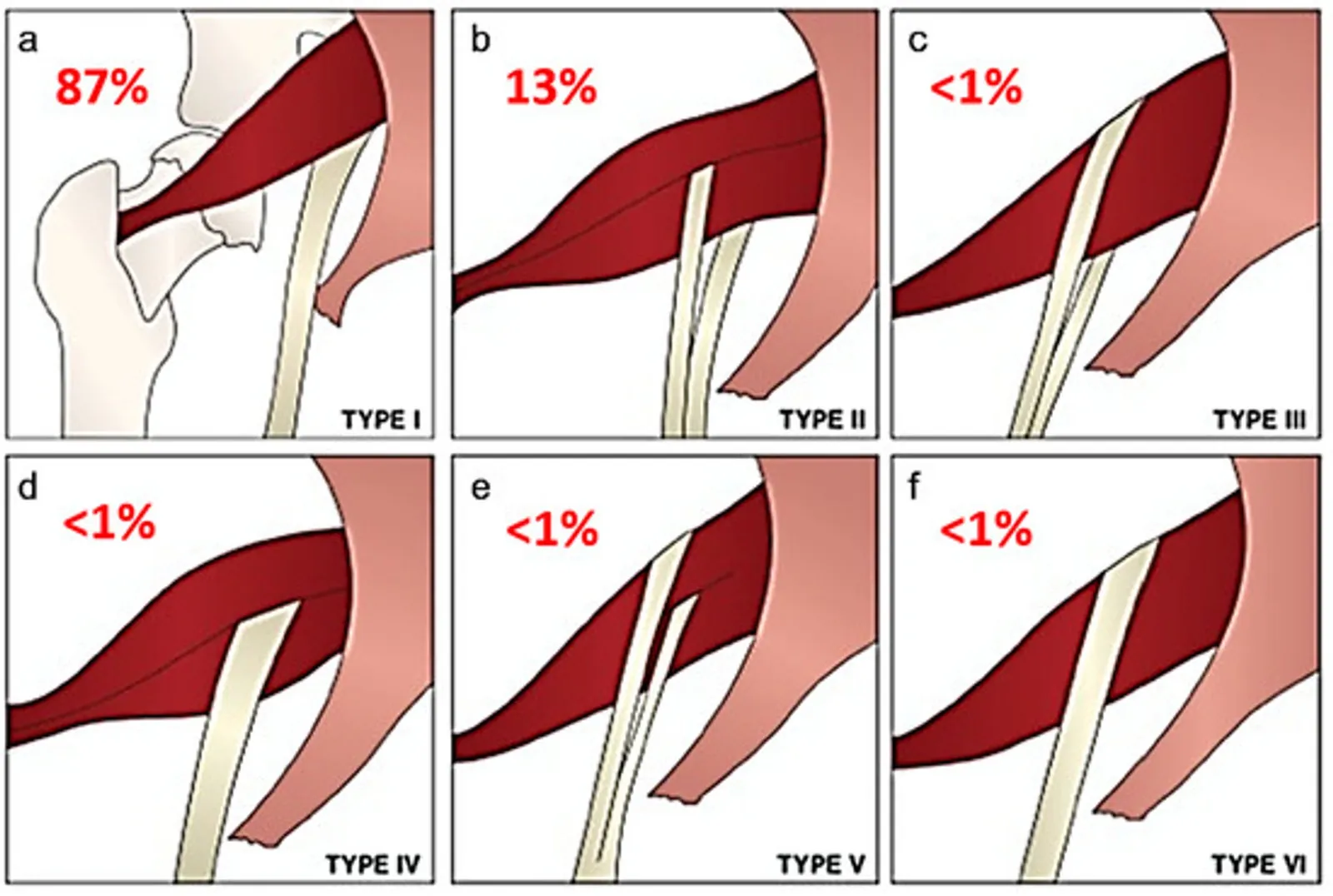
It also plays a role in stabilising the hip and the sacroiliac joint. Several anatomical variations in the course of the sciatic nerve have been described, and some predispose to the occurrence of the syndrome.
Causes of piriformis muscle syndrome
- Muscular contracture.
- Muscular hypertrophy.
- Anatomical anomaly.
- A cyst or tumour (rare).
- Inflammation.
Triggering factors
Trauma or repeated microtrauma
Falls onto the buttocks and direct trauma can cause lesions or spasms of the piriformis muscle.
Muscular overuse
Running, cycling, prolonged sitting. Excessive use of the piriformis as an external rotator and abductor of the hip.
Surgery or intramuscular injections
Poorly performed injections in the buttock or surgical procedures may damage the muscle or the sciatic nerve.
Postural or skeletal factors
Lumbar hyperlordosis, sacroiliac dysfunction, scoliosis or postural disorders may disrupt the pelvi-femoral balance (for example: leg-length discrepancy, excessive femoral rotation).
Pregnancy
Ligamentous relaxation and postural changes can cause increased stress on the piriformis muscle and promote compression of the sciatic nerve.
Clinical diagnosis
Diagnosis relies above all on a rigorous clinical evaluation, after ruling out spinal causes of sciatica (disc herniation, lumbar spinal stenosis, etc.).
Commonly used clinical tests:
- FAIR Test (Flexion – Adduction – Internal Rotation).
- Freiberg test.
- Beatty test.
- HCLK manoeuvre (Heel Contra-Lateral Knee).
- Painful palpation in the buttock.
Additional investigations:
- Pelvic MRI: may reveal muscular hypertrophy or an anatomical conflict.
- Electroneuromyography (ENMG): may detect a conduction delay of the sciatic nerve.
Therapeutic management
Conservative first-line treatment — Osteopathy or physiotherapy:
- Piriformis muscle stretching.
- Muscle strengthening (isometric).
- Release of trigger points.
- Lumbo-pelvic mobilisation.
- Postural correction.
Injections:
- Ultrasound- or CT-guided injections of cortisone or anaesthetic.
- Botox injection.
Surgery (neurolysis or muscle release): as a last resort and rarely required.

Conclusion
Piriformis syndrome is a real, though long-debated, pathology. Its recognition relies on sound anatomical knowledge, thorough clinical analysis and individualised management. Osteopathy, combined with specific exercises and correction of postural factors, achieves symptom resolution in the majority of cases.
Frequently asked questions (FAQ)
What is piriformis syndrome?
Piriformis syndrome is a contracture or inflammation of the piriformis muscle (located deep in the buttock) that can compress the sciatic nerve. It causes buttock pain that sometimes radiates into the leg, often mistaken for sciatica of lumbar origin.
How does osteopathy treat piriformis syndrome?
Osteopathy uses deep muscular release techniques, mobilisations of the hip and sacrum, and piriformis stretching to reduce compression of the sciatic nerve. 3 to 5 sessions are generally sufficient to achieve significant improvement.
How can you differentiate piriformis syndrome from lumbar sciatica?
Piriformis syndrome causes buttock pain aggravated by prolonged sitting and hip rotation, without associated low back pain. Lumbar sciatica is accompanied by lower back pain and is linked to disc or vertebral joint compression.
What are the causes of piriformis syndrome?
Causes include: prolonged sitting (wallet syndrome), direct trauma to the buttock, muscular hypertonia linked to sacroiliac dysfunction or gait imbalance. Athletes (runners, cyclists) are particularly affected.