Tendinopathy: causes, symptoms and treatment
Pathophysiology and treatment of tendinopathy
Tendinitis refers to inflammation of the tendons, the fibrous structures that connect muscles to bones. It occurs primarily after repetitive movements or excessive stress on a joint region, and may affect various parts of the body (shoulders, elbows, wrists, knees, heels, etc.). Sporting activities, repetitive occupational movements, and the natural ageing of the tendons, are frequent causes of this condition. Tendinopathy is a common musculoskeletal condition, particularly in athletes and manual workers.
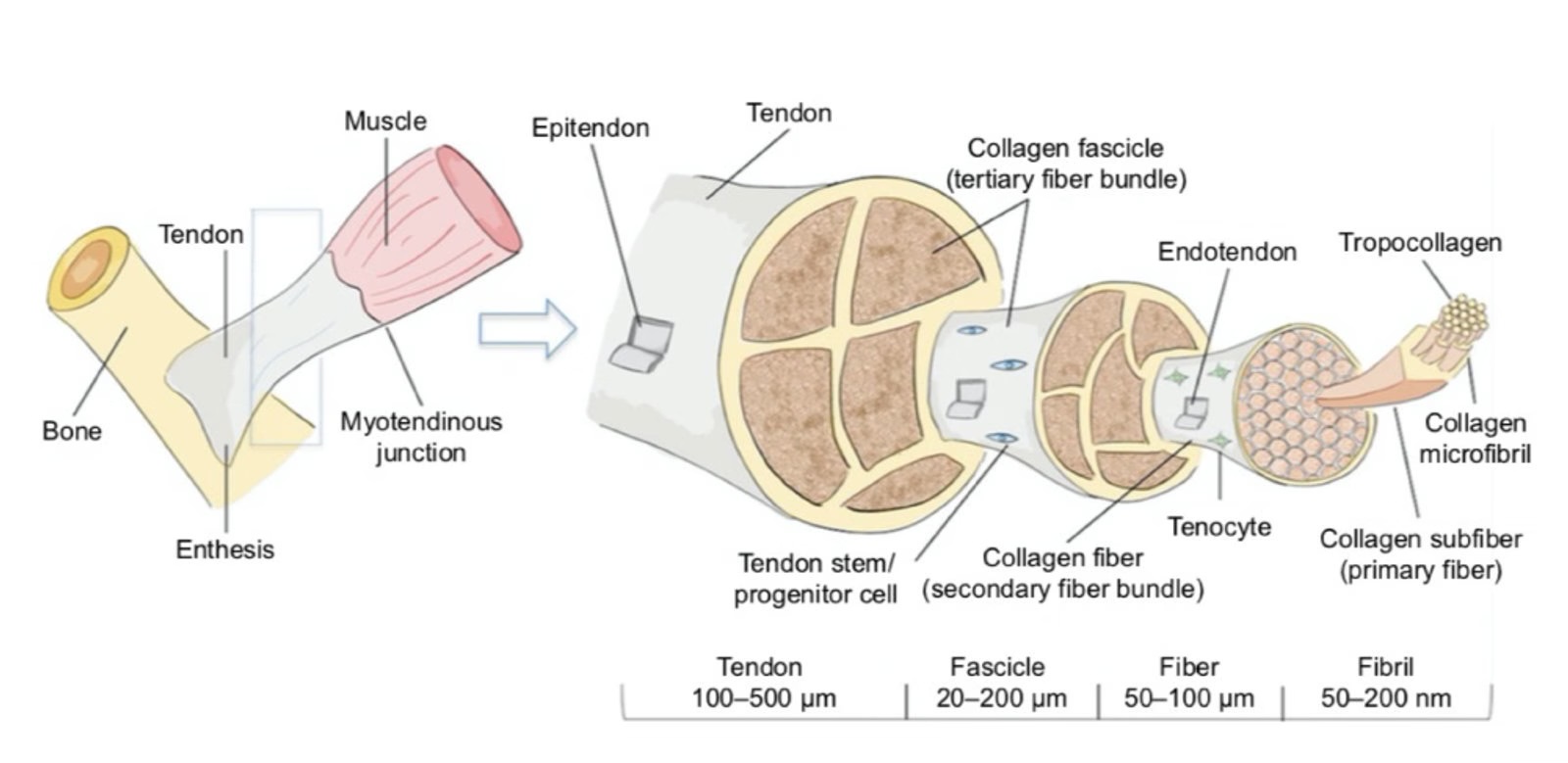
Tendons are dense connective tissues composed mainly of collagen fibres, which give them both strength and elasticity. Their principal role is to transmit the force generated by the muscles to the bones, thereby facilitating joint movement. They are poorly vascularised, which explains their tendency to heal slowly when they are damaged.
Pathophysiological mechanisms
Tendinitis is characterised by structural and functional changes in the tendons. The pathological mechanisms include:
- Repeated microtrauma: Repetitive movements or mechanical overload cause microtears in the tendon fibres. If the microtrauma is repeated without sufficient recovery time, local inflammation develops.
- Collagen degeneration: Following trauma, there may be an alteration in the production and organisation of the collagen fibres. This leads to a disorganisation of the tendon, known as degenerative tendinopathy.
- Biochemical and cellular factors: Inflammatory mediators, such as pro-inflammatory cytokines (for example, IL-1β, TNF-α) and proteolytic enzymes, are released in response to the lesions. They contribute to the degradation of the tendon's extracellular matrix.
The term tendinopathy is often used today to describe the full range of tendon disorders, because inflammation (the suffix "-itis") is not always present in chronic tendinopathies, where degeneration often predominates over inflammation.
Treatment of tendinopathy
Treatment of tendinopathy aims to reduce pain, limit inflammation (if present) and restore the functionality of the tendon. Therapeutic options include:
- Rest and modification of activities: Rest is often recommended to avoid aggravating the tendinopathy. In some cases, the ergonomics at work or in daily activities must be adapted to limit repetitive movements.
- Anti-inflammatory therapies: Non-steroidal anti-inflammatory drugs (NSAIDs) are frequently prescribed to ease pain and inflammation. In severe tendinopathies, corticosteroid injections may be considered, but these remain controversial as they may weaken the tendon over the long term.
- Rehabilitation and specific exercises: A rehabilitation programme aimed at strengthening and stretching the affected muscles and tendons is often prescribed. Eccentric exercises, which lengthen the tendon under tension, have shown particular effectiveness in the rehabilitation of chronic tendinopathies.
- Surgery: If conservative treatments fail, surgery may be considered to remove damaged tendon tissue or repair ruptures.
Other complementary treatments
- Ultrasound and shockwave therapy: These techniques are sometimes used to stimulate healing and reduce pain in chronic tendinopathies.
- PRP (platelet-rich plasma) injection: PRP is a promising method, using the growth factors contained in platelets to promote tendon regeneration.
Contribution of manual therapy and osteopathy in the treatment of tendinopathy
Manual therapy brings together a set of techniques aimed at relieving musculoskeletal pain through specific manipulations and mobilisations of the soft tissues and joints. In tendinopathy, several approaches have shown their effectiveness:
- Deep transverse friction massage: This type of massage is often used to increase blood flow at the tendon and stimulate tissue repair. It can also reduce inflammation by mobilising fluids and reducing oedema.
- Joint mobilisations: Manipulations of adjacent joints can reduce the mechanical stresses on the affected tendon and improve joint mobility.
The osteopath will seek to identify and treat the mechanical imbalances that may have contributed to the onset of the tendinopathy:
- Correction of joint dysfunction: A reduction in joint mobility may increase the stress on certain tendons. For example, a dysfunction of the cervical or thoracic spine could affect the tendons of the shoulder.
- Reduction of muscular tension: The osteopath uses manual techniques to release muscular tension, thereby improving vascularisation and reducing the mechanical load on the tendon.
- Global work on the myofascial chains: Osteopathy aims to rebalance not only the affected area, but also the body as a whole, taking into account the connections between the different muscular chains and fasciae.
Effectiveness and limitations
Several studies have shown the effectiveness of manual approaches in reducing pain and improving function in tendinopathies. However, these techniques must often be combined with an active rehabilitation programme to obtain lasting results. Furthermore, it is essential to treat the underlying cause of the tendinopathy (postural imbalance, mechanical overload, etc.) to prevent recurrence.
Conclusion
Tendinopathies are common conditions resulting from microtrauma and mechanical overload of the tendons. Their treatment relies primarily on a conservative approach including rest, anti-inflammatories and rehabilitation. Manual therapy and osteopathy can provide valuable support by improving mobility, reducing tension and promoting tendon regeneration. It is however crucial to adopt a multidisciplinary approach to maximise the chances of recovery and prevent recurrence.
Frequently asked questions (FAQ)
How does osteopathy treat tendinopathy?
Osteopathy identifies and corrects the biomechanical imbalances that overload the tendon (poor joint alignment, excessive muscular tension). It combines myofascial techniques, mobilisations and eccentric exercise advice to support tendon healing.
What is the difference between tendinitis and tendinopathy?
Tendinitis refers to acute inflammation of the tendon (often after trauma). Tendinopathy is a broader term that includes chronic degenerative tendon lesions, which are more frequent and often without classic inflammation. Treatment differs according to the stage.
How long does tendinopathy take to heal with osteopathy?
An acute tendinitis that is well managed heals within 4 to 8 weeks. Chronic tendinopathies require 3 to 6 months of treatment combining osteopathy, eccentric exercises and modification of training load.
Should sport be stopped in the case of tendinopathy?
Not necessarily. Reducing the load and adapting training are often sufficient. Complete rest may even slow tendon healing. Your osteopath will guide you on the optimal management of your activity load.